INTRODUCTION
Yersinia enterocolitis may present with gastrointestinal manifestations such as diarrhea, abdominal pain. Gastrointestinal symptoms may mimic inflammatory bowel disease (IBD), especially Crohn’s disease (CD). The pathogenesis of CD is multifactorial [1] and the association between IBD and gastrointestinal chronic inflammatory process have been suggested, but not confirmed [2–4]. Hereby, we described a case of a child with terminal ileitis due to Yersinia enterocolitica infection, presenting with intussusception mimicking CD.
CASE REPORT
A 6-year-old boy with chronic abdominal pain visited the emergency department with acute right-sided abdominal pain that suddenly worsened, and was referred to the pediatric department. He had no significant family or medical history. The abdominal pain was developed suddenly, localized at the right upper quadrant with a numeric rating scale of 8, and recurred at frequent intervals. He had diarrhea with Bristol stool scale of 5 to 6.
His body temperature was 36.9°C, heart rate was 100 beats/min, blood pressure was 120/80 mm Hg, and respiratory rate was 23 breaths/min. There was diffuse abdominal tenderness on the right upper quadrant but no palpable mass was palpated. Laboratory tests showed elevated white blood cell counts of 16,280 cells/μL, neutrophil counts of 13,860 cells/μL, erythrocyte sedimentation rate of 38 mm/hr, and C-reactive protein level of 2.26 mg/dL. He had hemoglobin level of 10.4 g/dL, hematocrit of 31.6%, ferritin of 14 ng/mL, iron of 17 μg/dL, total iron binding capacity of 426 μg/dL, which suggest iron deficiency anemia. Albumin, blood urea nitrogen, and creatinine levels were normal and interferon γ release assay were negative. Stool calprotectin level was elevated to 3,000 mg/kg.
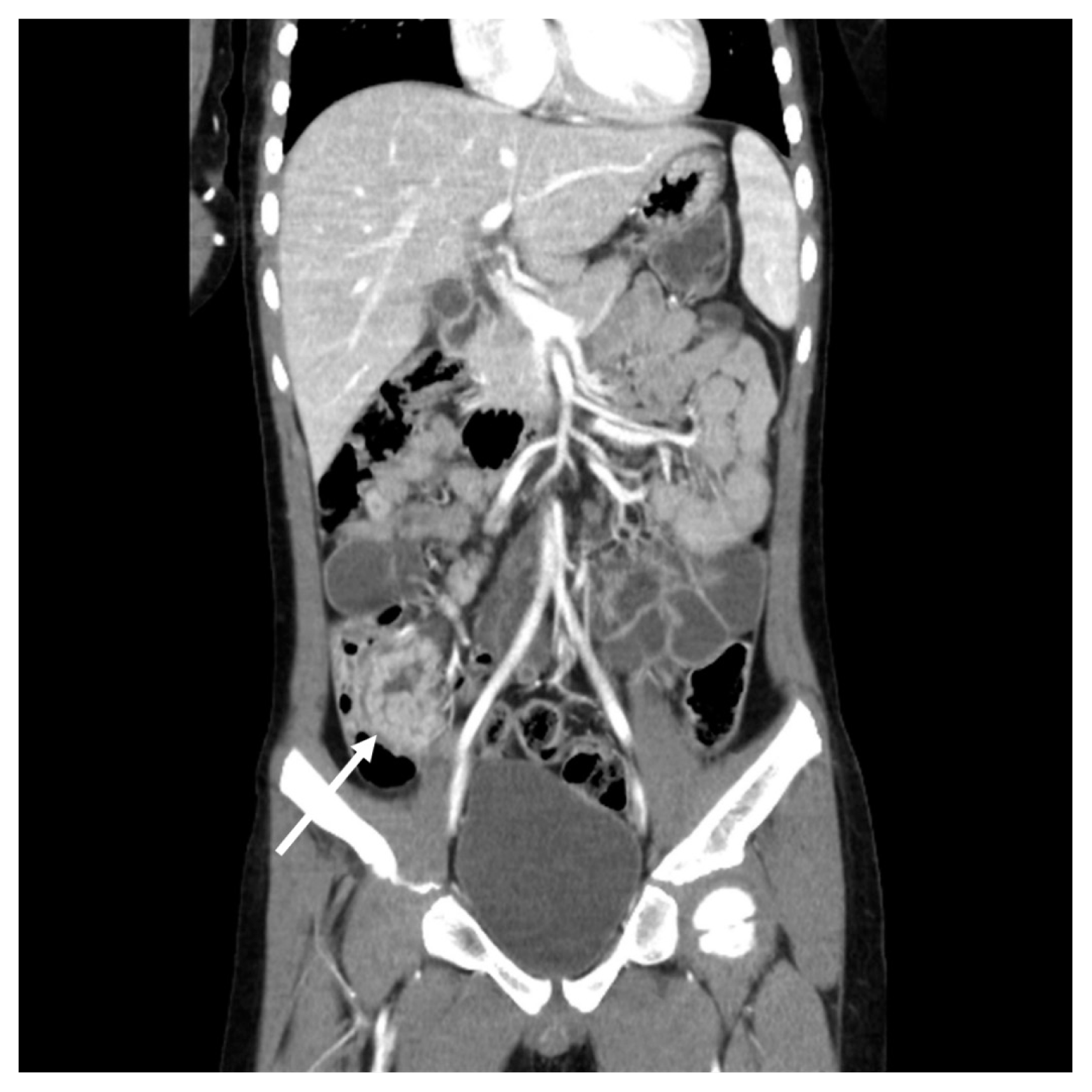
Ultrasound revealed target like lesion at the right lower quadrant. We diagnosed the patient with ileocolic intussusception. An air-reduction was performed on the day of admission, relieving colicky abdominal pain after the procedure. Diffuse abdominal pain, diarrhea, and low-grade fever were remained. Since intussusception is not common in 6-year-old child, we decided to perform abdomen computed tomography (CT). Abdomen CT showed thickening through terminal ileum, cecum, proximal ascending colon, and the polypoid lesion was suspected in the terminal ileum (Fig. 1).
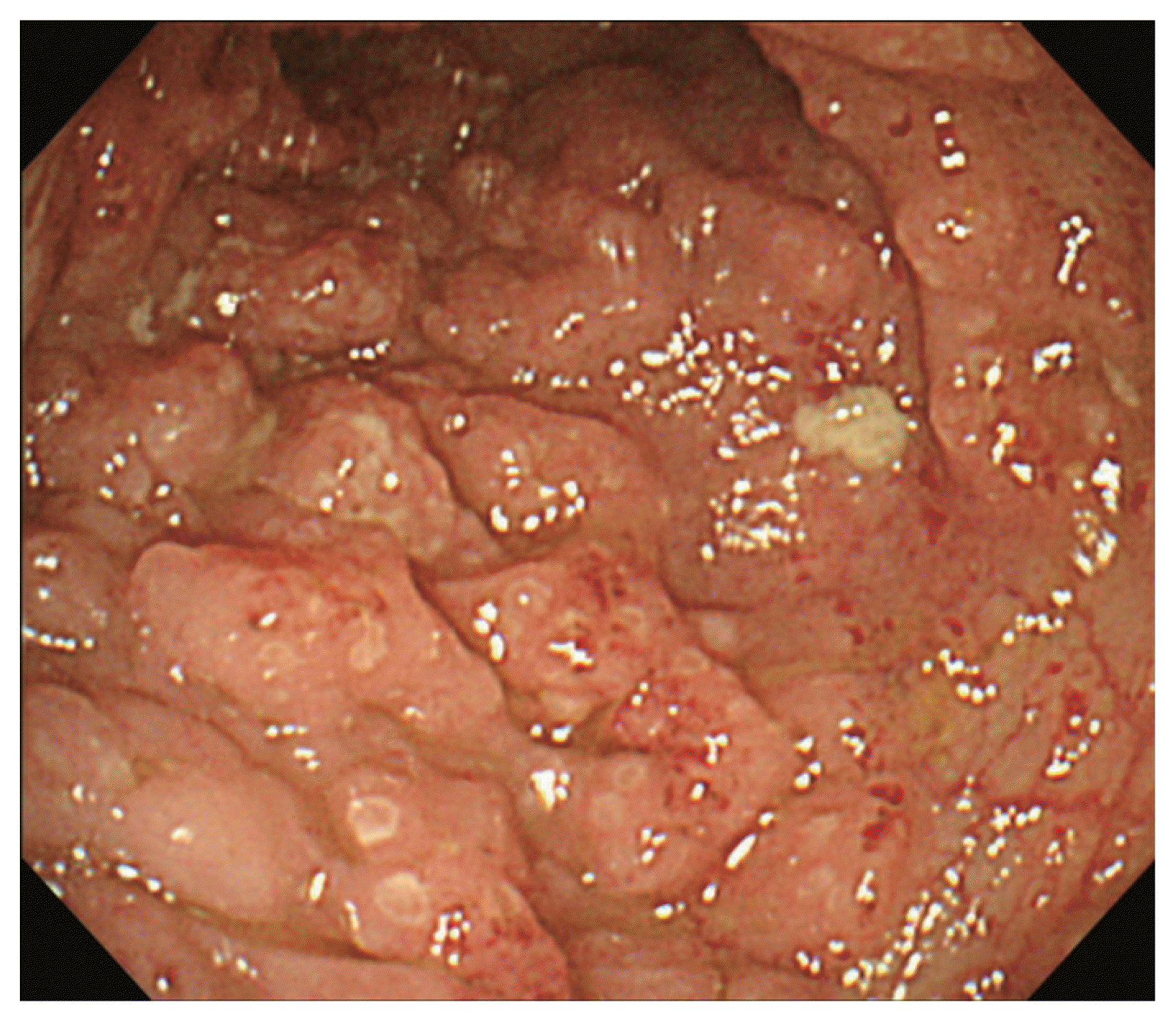
In the suspicion of IBD or polyp of the terminal ileum, we decided to perform endoscopy. The examination revealed the presence of a few small-sized ulcers in descending colon and cecum, and multiple aphthous ulcers in the terminal ileum in colonoscopy (Fig. 2). Pathology finding was chronic inflammation with cryptal distortion, which was consistent with a diagnosis of CD. These findings were consistent with the diagnosis of CD, A1-L3-B1 based on the Montreal classification. Exclusive enteral nutrition (EEN) and peroral mesalazine were commenced. On the 9th day after admission, stool bacteria multiplex real-time polymerase chain reaction (multiplex RT-PCR) revealed Yersinia enterocolitica infection. EEN and oral mesalazine were discontinued and supportive management was provided. His symptoms and signs improved gradually over 7 days. The patient was discharged on the 11th day after admission. Since CD was not yet completely ruled out, follow-up colonoscopy was scheduled. At the 2 months of follow-up, colonoscopy did not reveal any significant findings such as inflammation or ulcers. His calprotectin was normalized to 33 mg/kg. The patient did not suffer any signs and symptoms such as abdominal pain or diarrhea during 2-year follow-up. This case report was approved the institutional review board of Soonchunhyang University Bucheon Hostpiatl (IRB approval no., 2019-08-005). The patient provided written informed consent for the publication of clinical details and images.
DISCUSSION
This case report demonstrates a child of Yersinia enterocolitica ileitis accompanied by intussusception, which was similar to CD. Delayed diagnosis of Yersinia enterocolitis was due to slow output of stool examination and his presentations. The patient had chronic abdominal pain before the acutely aggravated severe abdominal pain which was consistent with CD, but turned out to be functional abdominal chronic pain without red flag signs. Furthermore, colonoscopy and biopsy also supported with CD with chronic inflammation and crypt distortion. There are few reports compare the endoscopic findings and fecal calprotectin between the acute phase of infection and the recovery phase after conservative treatment.
The etiopathogenesis CD is multifactorial with various environmental, genetic, immune-mediated, and gut microbial factors. Although the association between IBD and gastrointestinal infection such as Yersinia have been suggested, the mechanisms involved in the pathogenesis of CD are still not clear. Baumgart and Carding [1] suggested that IBD is more common after gastrointestinal infections, and people with disease generally have higher concentrations of mucosal bacteria than healthy people do. Also, Lamps et al. [2] reported pathogenic Yersinia DNA in a series of CD patient samples and suggested that Yersinia might play a role in the pathogenesis of CD. A case of mesenteric adenitis caused by Yersinia in a patient subsequently diagnosed with CD of the terminal ileum has been previously reported [3].
Yersinia enterocolitica is a gram-negative bacillus with a worldwide distribution, causing a variety of clinical manifestations ranging from self-limited enteritis to life-threatening systemic infection. Signs and symptoms of Yersinia enteritis vary from mild fever, abdominal pain, and diarrhea to bloody stool and high fever. Yersinia enterocolitica enteritis can mimics appendicitis, intussusception, toxic megacolon, gastrointestinal perforation, and peritonitis that would require pediatric surgical treatment [5]. In our case of terminal ileitis mimicking CD subsequently diagnosed with Yersinia enterocolitis. Le Baut et al. [4] revealed Yersinia is found in the same proportions in the control patients and the CD patients, regardless of their clinical presentation and Yersinia could be found in inflammatory and non-inflammatory parts of the ileum in CD patients.
Differential diagnosis of terminal ileitis is sometimes extremely challenging, and not every inflammation of terminal ileum is CD. There are few case reports on patients, who are not CD, being misdiagnosed as CD [6–9]. Terminal ileitis may be caused by a wide variety of diseases. We compared previous cases report of terminal ileitis caused by Yersinia species misdiagnosed as CD with our case (Table 1).
Our case suggests that Yersinia enterocolitica infection should be included in the differential diagnosis of patient suspicious of CD. Although Yersinia enterocolitica enteritis may well mimics CD, other infectious causes of other possible conditions should be ruled out after careful examination and follow-up and evaluation for CD should be started carefully after infectious enteritis has been ruled out in acute presentation with or without chronic symptoms.