INTRODUCTION
Cervical lymphadenopathy can be developed from various causes such as viral infection, bacterial infection, Kikuchi-Fujimoto disease (KFD), tuberculosis (TB), malignancy, and reactive changes [1]. Among these, KFD is a benign, self-limited syndrome characterized by cervical lymphadenopathy, fever and malaise that occurs predominantly in young people [2]. The etiology of KFD is unclear. The association of KFD and malignancy is also seldom discussed.
In patients who have malignancy, metastatic lymphadenopathy is possible. But it is rare that other concomitant diseases are in the same lymph node [3-9]. There have been some case reports related to concomitant two other diseases in a lymph node [3,5,8,10]. To our best knowledge, however, there is no case report of KFD and papillary thyroid carcinoma combined in a single lymph node. Here, we report a case of a 38-year-old man who has undergone surgical biopsy for recurrent cervical lymphadenopathy and were diagnosed with coexisted KFD and thyroid cancer in a lymph node.
CASE REPORT
A 38-year-old man was admitted on July 4, 2010 with a history of gradually worsening right cervical lymph node enlargement for a week. He did not have any past medical history and take medicine. He did not present any constitutional symptoms. On physical examination, non-tender, fixed lymph nodes were palpable at the right posterior neck. White blood cell count (WBC) was 2,550/μL (normal value, 4,000 to 8,000/μL), platelet count was 203×103 /μL (normal value, 150 to 450×103 /μL), lymphocyte proportion was 51.4% (normal value, 19% to 48%), aspartate aminotransferase, alanine aminotransferase was normal with 20 IU/L (normal value, 9 to 39 IU/L), 22 IU/L (normal value, 5 to 45 IU/L), and C-reactive peptide (CRP) was 1.8 mg/L (normal value, 0 to 3.0 mg/dL). Free T4 was 1.10 ng/dL (normal value, 0.89 to 1.76 ng/dL), thyroid-stimulating hormone (TSH) was 2.59 μIU/mL (normal value, 0.550 to 4.780 μIU/mL), and thyroglobulin (Tg) was 1.2 ng/mL (normal value, 0 to 35 ng/mL). Contrast enhanced neck computer tomography (CT) showed 2- to 6-mm-sized, round, multiple hypodense lesions in the right upper thyroid lobe and 4- to 10-mm-sized, irregular, rim enhanced multiple enlarged lymph nodes in ipsilateral internal jugular chain (IJC) (Fig. 1A, B). Fine needle aspiration (FNA) was done targeting the right thyroid mass. The pathologic finding was papillary thyroid carcinoma on thyroid mass. Total thyroidectomy and central neck dissection (CND) were performed and multifocal papillary thyroid carcinoma with lymph node metastasis (stage III, T2bN1aM0) was diagnosed (Fig. 1C). He took radioactive iodine therapy and had been treated with levothyroxine 0.2 mg. Eight months after the surgery, follow-up 131I whole body scan did not show any hot uptake and Tg was within normal range.
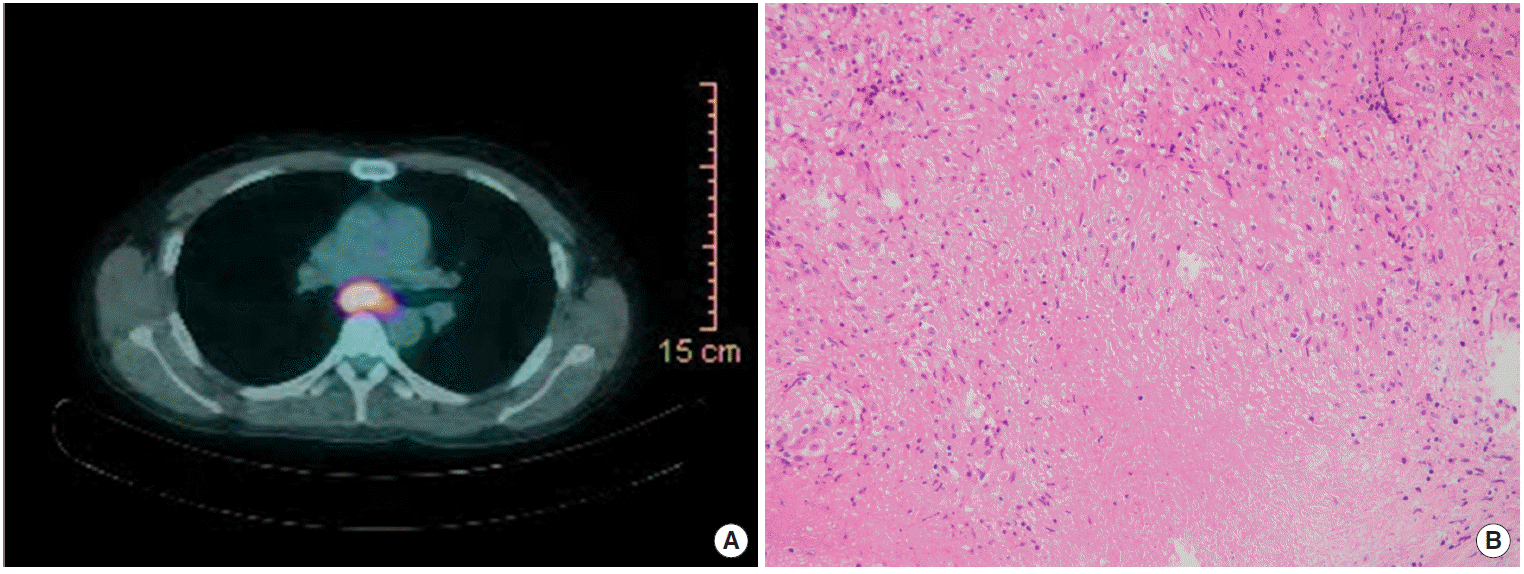
One year after the total thyroidectomy with CND, the patient started to complain of intermittent fever up to 38.3°C with chill, dry cough, and night sweat. On physical examination, about 1-cm-sized right supraclavicular lymph node was palpable and no other abnormal findings were found. The lymph node was nontender and firm and was presented with overlying erythema. The laboratory data showed elevated CRP as 64.7 mg/L and normal WBC as 4,300/μL. Thyroid profile was normal as the following results: free T4 1.60 ng/dL and TSH 1.67 μIU/mL. There was no abnormal finding with the chest X-ray. On chest CT, multiple lymph nodes enlargement appeared in the right supraclavicular, right paratracheal, and subcarinal area. The lymph nodes were 4- to 14-mm-sized, round-shaped, and peripheral rim enhanced with central necrosis. 18F-fluorodeoxyglucose (FDG) positron emission tomography (PET)/CT was done in which there were hypermetabolic lymph nodes in right neck, supraclavicular, and mediastinal area (Fig. 2A). FNA on right IJC lymph node was done and just atypical cells were reported. Because the central necrosis was more prominent in mediastinal area on CT image, paratracheal lymph nodes biopsy was done by a thoracic surgery doctor for definite diagnosis. Through microscopic examination, chronic granulomatous inflammation with caseous necrosis was observed. This was consistent with TB (Fig. 2B). The result of nested polymerase chain reaction (PCR) for mycobacterium tuberculosis was also positive. He started anti-TB medication made up of isoniazide, rifampin, pyrazinamide and ethambutol. After six months of treatment, right lower neck lymph nodes were more enlarged on physical examination despite the anti-TB therapy. Considering the paradoxical response, anti-TB therapy was continued further three months. After finishing the anti-TB therapy for nine months, he took 18F-FDG PET/CT. Preexisting lymph nodes on left paratracheal disappeared, and lymph nodes on the right supraclavicular, right paratracheal, and subcarinal area decreased in size by about half to one third.
Nine months after the end of the anti-TB therapy, he visited the hospital due to fever, dry cough, sore throat, and generalized myalgia for two weeks. With the physical exam, about 1.5-cm-sized firm, fixed, and tender lymph node was newly palpable on the right posterior neck. Laboratory reports were as follows: WBC 2,760/μL, CRP 33.3 mg/L, TSH 0.007 μIU/mL, free T4 1.48 ng/dL, and Tg <0.100 ng/mL. On 18F-FDG PET/CT, right supraclavicular, paratracheal, and subcarinal lymph nodes increased comparing with the previous 18F-FDG PET/CT. In addition, both axillary and retroperitoneal lymph nodes enlargements were newly observed (Fig. 3A). Excision biopsy was done on the right cervical and right supraclavicular lymph node. Microscopically, the lymph nodes were composed of focal, well circumscribed subcortical necrotizing lesions with abundant karyorrhectic debris, compatible with KFD (Fig. 3B, C). On immunohistochemical stain, there were many histiocytes with immunoreactivity for CD68 and myeloperoxidase. Simultaneously, microscopic foci of metastatic papillary carcinoma were identified in the same lymph node (Fig. 3B, D). TB was not suspected in microscopic finding and TB nested PCR was negative. The final diagnosis was KFD combined with metastatic papillary carcinoma. Because the malignant pathologic finding was just a small portion of lymph node and he already had taken a total thyroidectomy and lymph node dissection, we decided to continue the levothyroxine medication without further radioactive iodine therapy or operation under the discussion with endocrinologist. Instead, methylprednisolone and non-steroidal anti-inflammatory drugs were added to treat the KFD. Three months later, hypermetabolic lymph nodes at mediastinal and axillary area were completely diminished in 18F-FDG PET/CT and his symptoms have been completely resolved without recurrent symptoms.
DISCUSSION
Metastatic lymphadenopathy is possible in patients with malignancy. But it is rare that other concomitant diseases are in the same lymph node [3-9]. The case of lymphoma and localized Castleman’ s disease within the same lymph node was reported [11]. This could be possible because localized Castleman’s disease has potential to develop into lymphoma, sarcoma, and carcinoma. Also the coexistence of TB and malignancy such as lymphoma, leukemia, and solid tumor has been discussed before [5]. This can be possible due to the impaired cell-mediated immunity that is affected by immunosuppressive therapy or malignancy itself. This coexistence can be possible subsequently. Incidence of TB in patients who have lymphoma is much higher than general population [12].
KFD is a self-limited and benign disease characterized by cervical lymphadenopathy, fever, and malaise. The etiology of KFD is unclear but some have reported infectious and autoimmune etiologies [2]. It means that KFD can occur more frequently under immunosuppressive condition like TB. But there is no accurate reported study about mechanism and relationship.
Our case is about a patient who had twice-recurrent cervical lymphadenopathy. Initially, the thyroidectomy and neck dissection revealed them as metastatic papillary carcinoma. One year after the surgery, he complained of cervical lymphadenopathy and fever. Because he had thyroid cancer history, the possibility of recurrence could not be ruled out. Through the surgical biopsy, he was diagnosed with TB lymphadenitis. After the anti-TB therapy, cervical lymphadenopathy was unfortunately developed again. Surgical biopsy confirmed the final diagnosis as KFD accompanied by metastatic papillary thyroid cancer. Interestingly, KFD and metastatic thyroid cancer coexisted in one lymph node and twice-recurrent cervical lymphadenopathy were diagnosed differently from each other. The pathology could be the results of remained thyroid cancer or incidental finding. However, it might be meaningful case. Studies and cases about researching cause of KFD have been reported but mostly limited to virus or autoimmune disease. As mentioned, under the immunosuppressive condition virus may activate KFD more frequently. However only one case have been reported the coexistent KFD and carcinoma until now [13]. The association between KFD and malignancy is obscure and there is no reported study. Our case suggests the need for further studies to reveal the relationship of KFD and malignancy as well as KFD and TB. In addition, which treatment should be chosen is another dilemma. Decision to treat both two disease or not is always considered and wise choice is needed.
The coexistence of two other diseases is rare but diseases that the association have not been unproven can coexist, the possibility of other concurrent diseases have always to be kept in mind especially in patients with malignancy history.