INTRODUCTION
Hepatocellular carcinoma (HCC) is the 5th most common cancer in South Korea. And it is the 4th most common cancer in Korean men and 6th most common cancer in Korean women [1]. Most preferred treatment is surgical resection. Even though that, many patients with extended disease or decreased liver function are inappropriate for surgery.
Transcatheter arterial chemoembolization (TACE) is suitable treatment for these patients. Recently TACE is commonly used treatment method for HCC, because of its execution time saving and wide indications. It could be applicable for patients with distant lesions from each other, huge sized tumor or decreased liver function. But there are some complications. The risk of embolic events caused by therapeutic embolic materials is one of those in the treatment.
CASE REPORT
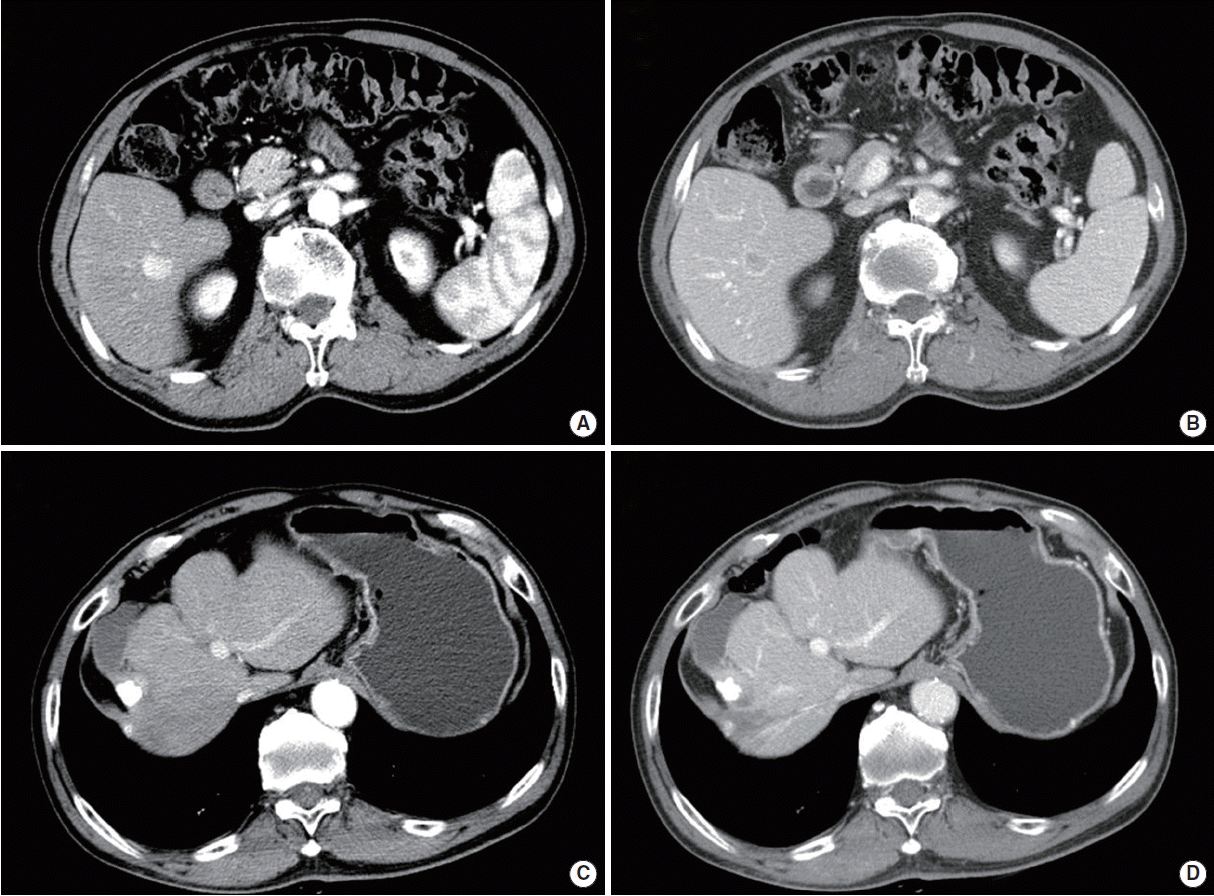
A 61-year-old man, who already had been treated with 5 times of TACE, went to undergo 6th procedure. He was treated by TACE for 6 times during 6 years. Last TACE was planned to be done for marginal recurrence and remnant viable portion of HCC at S6 and S8 (Fig. 1).
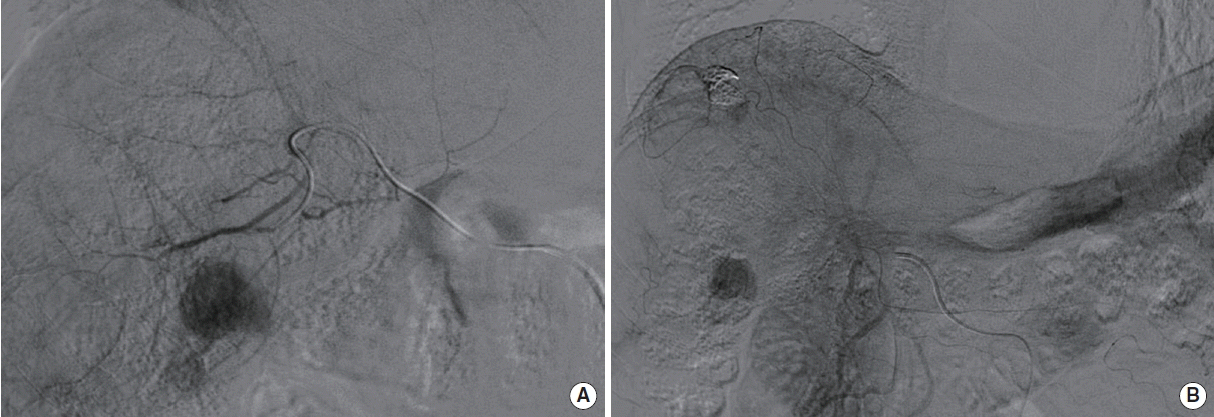
During the procedure, adriamycin (50 mg) and lipiodol (5 mL) mixture was infused via feeding branch of right hepatic artery. No gelfoam embolization was done due to injured intrahepatic arteries (Fig. 2). Immediately after the TACE, he complained of abdominal pain in right-upper-quadrant. And next day of procedure, the patient felt nausea and chilling sense. Fever sustained three days and body temperature rose to 39°C. Abnormal liver functions were seen. Serum levels of aspartate aminotransferase and alanine aminotransferase were checked up to 179 mg/dL (normal value, 5 to 40 IU/L) and 231 mg/dL (normal value, 0 to 40 IU/L). White blood cell count was elevated to 11,490/uL (normal value, 4,000 to 10,000/μL). Antipyretics and analgesics were administered to him. The treatment made symptoms and fever decreased but not removed. He was discharged 6th post-procedural day.
In out-patient clinic, still he was suffering from that pain. And then we took the follow-up computed tomography (CT) image for response evaluation and there were abnormal findings on gallbladder. Gallbladder was distended and linear air density was seen below the enhanced thick wall (Fig. 3). These clinical signs and symptoms suggested gallbladder infarction caused by the embolic event during chemoembolization. Then we used oral antibiotics (cefditorene) and analgesics (acetaminophene) for 12 days. After the treatment, the patient felt better, and some improvement was seen in CT image, taken at 6th week after the event. CT image showed decreased volume of gallbladder infarction and disappearance of air bubbles. Also patient’s symptoms are resolved.
DISCUSSION
HCC presents multi-centric carcinogenesis and intrahepatic metastasis, because most of HCC cases have underlying liver diseases (e.g., chronic viral hepatitis, alcoholic liver disease). HCC frequently recurs after primary treatment and it is even often multifocal. TACE has been widely used as a treatment for multifocal HCC in patients, in whom curative treatment is difficult to perform [2]. Also it can be applied to patients with poor liver function or multiple lesions. Thus the Barcelona Clinic Liver Cancer staging system recommends TACE for intermediate-stage HCC (four or more tumors), and the Japan Society of Hepatology consensus recommends TACE for patients with a Child-Pugh score A or B, tumor diameter of more than 3 cm, or four or more tumors [3,4].
Therapeutic effect of TACE is based on the phenomenon, which is that, advanced HCCs are fed only by the hepatic artery and is intended to embolize the distal portion of the hepatic artery [5]. In contrast, it contains aspect of risk such as systemic embolization.
In the past, some cases were reported. They referred to gallbladder infarctions caused by preoperative hepatic artery embolization with gelfoam. Preoperative hepatic artery embolization is performed to decrease the vascularity and size of the HCC before operation and to prevent intrahepatic spread during surgery [6,7]. In our case, surgery was not considered and we use only lipiodol without gelfoam. Not only gelfoam, but also Lipiodol has embolic risk. Pulmonary, cerebral, and biliary embolisms caused by lipiodol were reported [5,8,9]. Sometimes, embolic event is only a mild feature, but some reports mention about biliary necrosis, which requires surgical treatment or some invasive interventions like percutaneous drainage [8]. When embolic material plugs the cystic artery, irreversible ischemic complication can be developed. Furthermore, compared to liver, the gallbladder is supplied from only cystic artery. So gallbladder is vulnerable to this ischemic event.
After TACE, nausea, vomiting, fever, and right upper quadrant pain are frequently present. This symptoms and signs are called as postembolization syndrome. It usually recovers spontaneously [5]. But this is similar to clinical features of the gallbladder embolism. Therefore, following-up of patient’s symptoms and laboratory values such as inflammatory markers is important to differential diagnosis and as in this case, image studies are useful.
Furthermore, this patient has recovered with only pharmacologic treatment. Early start and maintenance of antibiotics could have prevented for worsening of necrosis.